Table of Contents
ToggleCradle Cap in Babies: Top 5 Solutions
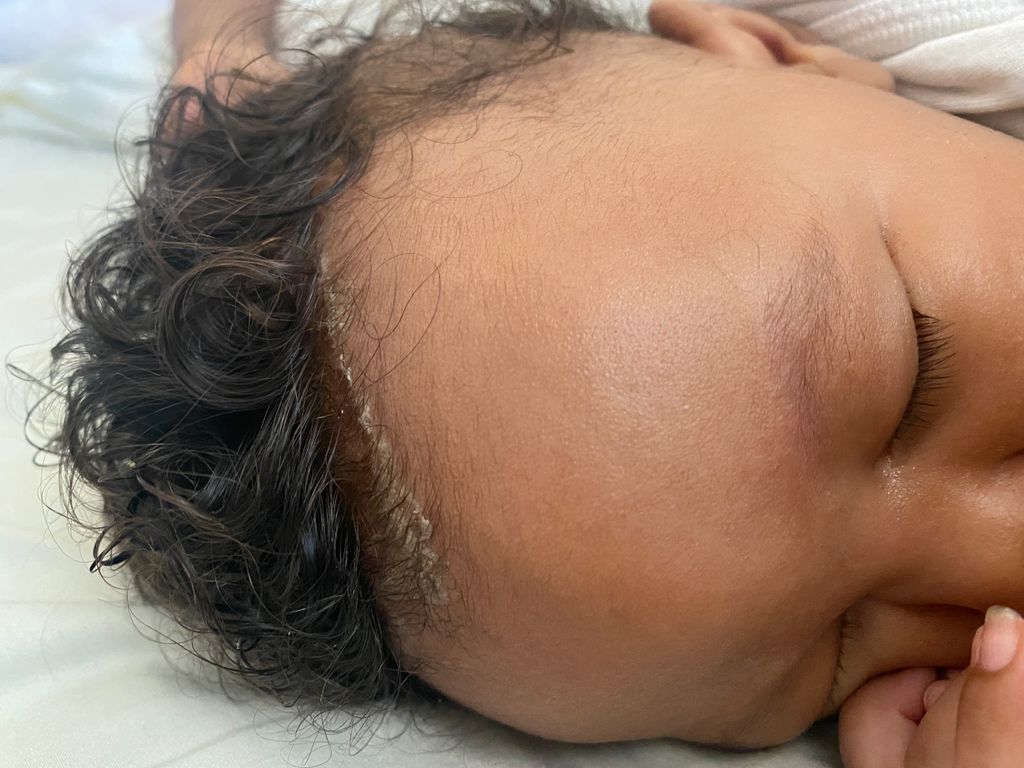
Cradle cap in babies seem to be a nightmare to parents, especially the first-time ones. The more they clean it, the more it seems to stay. What is cradle cap and what risk does it pose to babies?
According to research, at least 70% of babies get a cradle cap by 3 months. It is so common, so, don’t fret.
Do you want to know more about cradle cap? Read to the end.
What is a Cradle Cap?
Cradle cap is a skin condition that affects babies’ scalps, creating rough patches.
You can also call it crusta lacteal, milk crust, seborrheic dermatitis, crib cap, honeycomb disease, or pityriasis capitis.
Different babies develop this skin condition at different times, but it is predominant between one to three months. In some instances, the condition can stretch to 2 years.
Cradle cap is one of the issues that babies before turning two, as discussed in this post.
What Causes Cradle Cap in Babies?
There is so much mystery surrounding the causes of cradle cap in babies. The most commonly discussed is that the condition occurs due to excess oil production by the skin. The excess oil accumulates on the skin, combining with dead skin cells to create a thick layer on the scalp.
Another school of thought is that mothers can pass some hormones to the baby. The baby’s body may react to the hormones through the development of cradle cap.
Can a Baby Transmit Cradle Cap?
No. Cradle cap cannot be transmitted from one person to another.
What are the Symptoms of Cradle Cap?
A baby with cradle cap will manifest the following symptoms:
1. Hair Loss
In rare instances, cradle cap may lead to hair loss in the area affected. This should not worry you, since it grows back when the cradle cap goes away.
2. Change in Scalp Color
In some instances, babies with cradle cap develop a different skin color from the rest of the scalp. In some instances, it might appear ashy or yellow-like.
3. Greasy patchy scalp
Cradle cap will usually leave the baby’s scalp looking greasy. In severe instances, the greasy scalp might develop yellow or white patches.
4. Spread of Cradle Cap
In some instances, the cradle cap may spread to other parts of the body such as the armpits and ears.
How can You Diagnose Cradle Cap?
Diagnosing cradle cap is not rocket. A simple observation of the mentioned symptoms will tell you if the baby has a cradle cap.
How can You Treat Cradle Cap?
Once your dermatologist or pediatrician has diagnosed the baby with a cradle cap, they will prescribe these management or treatment tips:
- Wash the Scalp
The first step to treating cradle cap in babies is washing their scalp clean frequently. While washing the baby’s scalp, gently rub the scalp to remove all the extra oils.
It is also advisable to use unscented baby shampoo to wash the baby’s scalp. In my next article, I will attach a list of medicated shampoos that you can use to wash a baby with a cradle cap.
Note: Avoid shampoos whose ingredients are designed to treat dandruff.
- Brush the Scalp
Once you have washed and cleaned the baby’s scalp, the next step should be a gentle brush. Use a fine-tooth combi to brush the area with the cradle cap. With time, the scales will fall off with time.
- Apply a lubricant
Apply a baby-friendly lubricant to the scalp such as baby oil, petroleum jelly, or ointment. It is recommended that you apply the lubricant before using the hair brush on the baby’s scalp.
- Avoid picking the scales
Parental instincts might push you to pick the baby’s scales. However tempting the urge to pick the scales might be, avoid it since it could lead to re-infection.
- Apply Prescription Cream
If the baby’s scalp appears inflamed, apply a considerable amount of hydrocortisone antipruritic cream. Alternatively, you can apply ketoconazole cream to the scalp. Although these creams might not be effective in the long run, your doctor may recommend them.
When Should a Doctor Help You Manage Cradle Cap?
Although cradle cap is a common skin condition among babies, at times, it might need a doctor’s intervention. If your baby demonstrates one or several of these symptoms, see the doctor:
- Has an inflamed rash just behind their ears.
- Appears sickly.
- Is under 1 month old but already has blisters or pimples on their scalp.
- Their scalp smells bad.
- The rash spreads beyond to other parts of the body.
- Fluid or blood seems to ooze from the skin, especially the scalp.
FAQs on Cradle Cap
What is the difference between cradle cap and eczema?
Although cradle cap may be mistaken for eczema, there are notable differences.
First, cradle cap is usually greasier, thicker, and more yellow/brown than eczema.
On the other hand, eczema is itchier, pinkish or red, depending on the baby’s skin color. Additionally, babies with eczema have very sensitive skin, which is not the case with cradle cap.
How can I get rid of the cradle cap effectively?
- Wash the scalp daily.
- Brush the scalp gently and apply a lubricant.
- If the scalp is inflamed, apply a cream.
- Is it safe to pick up the scales?
- It is not safe to pick up the scales in babies with cradle cap.


